one day (part I)
This is a 3-part blog series I wrote about one 28 hour on-call shift at the Hospital of Hope. If the wifi works (which is a BIG if here in rural West Africa, I'll post all three this week.) *
It’s Saturday morning and I’m on call with a Family Practice doctor who’s visiting for a month from the United States.
We’ve rounded on our patients in pediatrics and maternity and medicine, and now we’re about to go into an isolation room to see our last patient.
We put on masks, gowns and gloves and enter the room, which called ISO 3, because it’s one of three isolation rooms we have for patients who have potentially contagious diseases.
My heart skips a beat when I see the patient. She’s a 22 year-old woman who’s 5’2” and a scant 83 pounds. Her eyes are yellow with jaundice, and there’s an oxygen mask on her face. She’s sitting up in bed, breathing rapidly, her thin chest heaving with each breath, as if it takes every muscle in her body to move air in and out.
We listen to her lungs, which sound congested. She has tenderness in her right upper quadrant, where the liver is located. Her lips are pale and when we press on her nail beds, it takes a few seconds for the blanching to go away. I look up at the monitor. Her heart is beating too fast — 140 beats a minute (normal is 60-100). Her oxygen saturation is 90% — which is low, especially since she’s getting the maximum amount of oxygen through the mask on her face.
We finish our exam in a few minutes, leave the room, remove our masks and gowns and gloves, and wash our hands thoroughly at the sink.
We sit down at the nurses’s station and flip through her chart. It’s her 4th day in the hospital. She was admitted for pneumonia and respiratory distress. We pull her chest x-ray up on the computer — and it looks awful. Her lungs are filled with infection.
She’s on several different I.V. antibiotics, but every day she gets worse.
“If we don’t figure out what’s wrong with her really fast, we’re going to lose her,” the doctor says, shaking his head.
At first, the medical team thought she had leptosporosis, a disease that’s transmitted by fresh water that’s contaminated with rat urine.
(It’s rainy season in Togo, and I think of the many puddles I’ve sloshed through on my walks through town. I make a commitment right then and there to scrub my feet every night to get all the animal urine off.)
But the woman is on the right antibiotic for leptosporosis, and she’s not getting better.
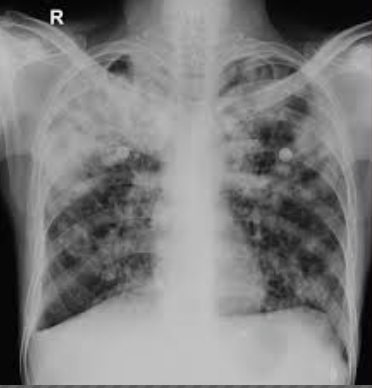
The only other disease we can think of that affects both the lungs and the liver is tuberculosis. They’ve done sputum samples on her, looking for TB, but they’ve been negative. Often sputum samples don’t provide enough organisms to show up on an analysis. In the U.S., a patient would have a bronchosopy where they stick a tube down into the lungs to get sputum for a culture, as well as a lung biopsy to confirm the diagnosis. But we don’t have any of those capabilities here.
A surgeon who has spent a lot of time practicing medicine in Africa walks over, and we show him the chest x-ray. “Oh yeah, that’s TB,” he says.
“How much does she weigh?” he asks me.
“83 pounds,” I said.
He nods his head. “There’s a reason they used to call this disease ‘consumption.’ It eats up your whole body.”
There are five antibiotics that treat tuberculosis. A patient has to be on at least three of them to treat the disease. Our hospital only has two.
There’s a government hospital in town that treats tuberculosis, but the problem is, we don’t have portable oxygen tanks. We only have oxygen that comes through a hose in the wall. If we take this woman off oxygen, she’ll die within minutes.
The more I think about the case, the faster my pulse goes.
This woman is going to die soon.
We know what she has and what she needs.
We can’t get her to the treatment center because we don’t have portable oxygen.
We can keep her here and give her oxygen, but only two of the three antibiotics she needs.
She’s on all the oxygen we can give her, and she’s still hypoxic.
Her body is wasting away.
Her lungs are giving out.
We’re running out of time.
She has a husband and two children.
This woman is dying on us.
There’s nothing we can do.
I was taking overnight call that night. Before the Family Practice doctor left for the night, I asked him, “If she codes, there’s nothing…?”
He shook his head sadly, and left.
As he was walking out the door, I got called into the woman’s room. Her oxygen was 85%. She was working even harder to breathe. Her upper abdominal pain was getting worse. She had a panicked look in her eyes.
Her parents were standing at the foot of her bed. Her husband was sitting on the floor. They were watching this woman struggle, and watching me to see if — and how — I could help her.
“Get her 4 milligrams of morphine and 2 milligrams of Valium,” I told her nurse. Tout suite.
We had turned a corner. I was no longer saving her life; I was helping her die. Morphine and Valium are two of the most commonly-used drugs in hospice. Morphine for pain, Valium for anxiety. And both meds are sedating, reducing the consciousness of the suffering patient.
I put my hand on the woman’s shoulder. “Can I pray for you?” I asked in French.
She nodded. Her husband and her parents nodded even more eagerly.
I prayed for her in English — because my vocabulary isn’t good enough to pray a full prayer in French.
“God, please be with my sister,” I said. “I pray for a miracle, that you would heal her and bring her back to a full, healthy life with her family.”
I paused and took a deep breath. Her monitor started dinging. I looked up and saw that her oxygen had dropped to 82%. I hit the “silence” button on the monitor.
“But if that’s not your will, and if it’s time for you to take this woman home…” my voice cracked. I took another breath. What would I want someone to pray for me if I was dying?
“Then I pray that you would be with her now, that you would comfort her, that you would help her not to be afraid, that you would help her not to suffer, that you would let your angels attend to her and carry her safely, gently Home.
“Comfort her loved ones as well, and help them to feel your presence and your love at all times.”
The nurse was back with the drugs.
“Amen,” I said.
The nurse administered the meds through the woman’s I.V. I stood there with my hand on her shoulder for a few minutes until her body relaxed, her eyelids grew heavy, and she laid her head back.
“There’s nothing we can do, except try to keep her comfortable,” I told her family in French. They nodded that they understood.
“I’m here all night if you need me,” I said as I left.